Michael A. Echteld PhD [1,2], Linda Tielen [1], Gabriëlle van de Graaf MD [1] and Michael Kolen PhD [1]
Michael Echteld’s e-mail: mechteld@prismanet.nl or ma.echteld@avans.nl.
[1] Prisma Foundation, The Netherlands; [2] Avans University of Applied Sciences
On this page you will find the article that accompanies the poster with the same title presented at the 2019 conference of the European Association for Palliative Care (EAPC). Download the poster in PNG format or as a PDF.
Download the article in PDF format here. The article text is also displayed below.
Background
Most people in The Netherlands have access to high quality palliative care—multidisciplinary total care aimed at patients’ quality of life when patients have limited life expectancies. All nurses and generalist physicians receive at least basic palliative care training. Nursing home staff is also well aware of palliative care principles. For patients with life expectancies of three months or less, hospice care is available in stand-alone hospices or units in nursing homes. In general, however, hospice care is only accessible to people who are aware of their life expectancies and who do not exhibit complex behaviour or behaviour experienced as disruptive or disturbing. Therefore, people with at least moderate intellectual disabilities, dementia, acquired brain damage, psychiatric problems, substance abuse problems and homeless people are often denied access to hospice care. This paper describes the patients of Balade, a hospice for people with limited access to hospice care.
People with intellectual disabilities, dementia, acquired brain damage, psychiatric problems, substance abuse problems and homeless people have in common that communication is usually more difficult than with people in the general public. Effort, experience and/or knowledge are required to learn about their symptoms, wishes and values. In addition, communicating aspects of illness and care to them is often difficult. For these reasons, regular hospices experience serious difficulties in providing optimal care for patients with these characteristics. Advance care planning, shared decision making, symptom assessment and care for symptom relief are viewed as highly challenging. They also experience admission of these patients to their hospices as a threat to the quality of care for the regular patients.
Hospice Balade, in the South of The Netherlands, was started as the only hospice specially for people with intellectual disabilities, dementia, acquired brain damage, psychiatric problems, substance abuse problems and homeless people. Balade is part of the Prisma Foundation, which is a care organisation for people with intellectual disabilities. Balade does not only provide care for Prisma clients but aims at the entire population in the region. Balade has 24/7 nursing and social staff, a dedicated hospice physician with a specialism in intellectual disabilities, a spiritual care counsellor, a psychologist, and access to physiotherapists, dieticians, occupational therapists, and speech therapists. All staff has experience with at least people with intellectual disabilities and is trained in palliative care. Balade has six beds.Balade is unique in The Netherlands. It opened its doors in January 2017 as an experiment. It was unknown then whether the intended population would be able to find its way to the hospice, and if they would, what their characteristics would be. In order to learn, reflect and improve the care provided in Balade, we collected data on patient illness and treatment characteristics, as well as narrative accounts of the care.
Methods
Data from all patients admitted to the hospice from January 2017 to February 2019 were collected. Patient, illness and treatment characteristics were derived from the patient records. Hospice staff was interviewed in order to identify instances of care crises, i.e., when symptoms could not be controlled. Descriptive statistics were performed in IBM SPSS Statistics version 25. Differences between groups were tested with the Chi-square, Mann-Whitney U and Kruskall-Wallis H tests. On admission, all hospice patients are informed that non-identifiable patient data may be used for care evaluation purposes.
Results
The first patient was admitted to Balade in February 2017. In total, 62 patients were admitted to the hospice. Eighteen patients were referred to the hospice by the Prisma Foundation (i.e., internal referral), and 44 were referred by various external organisations. Fifty-six patients died in the hospice. None of the patients died in crisis or with uncontrollable symptoms. A blow-out in the neck occurred in one patient due to a neck carcinoma, but the patient did not experience the blow-out consciously. Patients presented the staff with significant communication and social challenges.
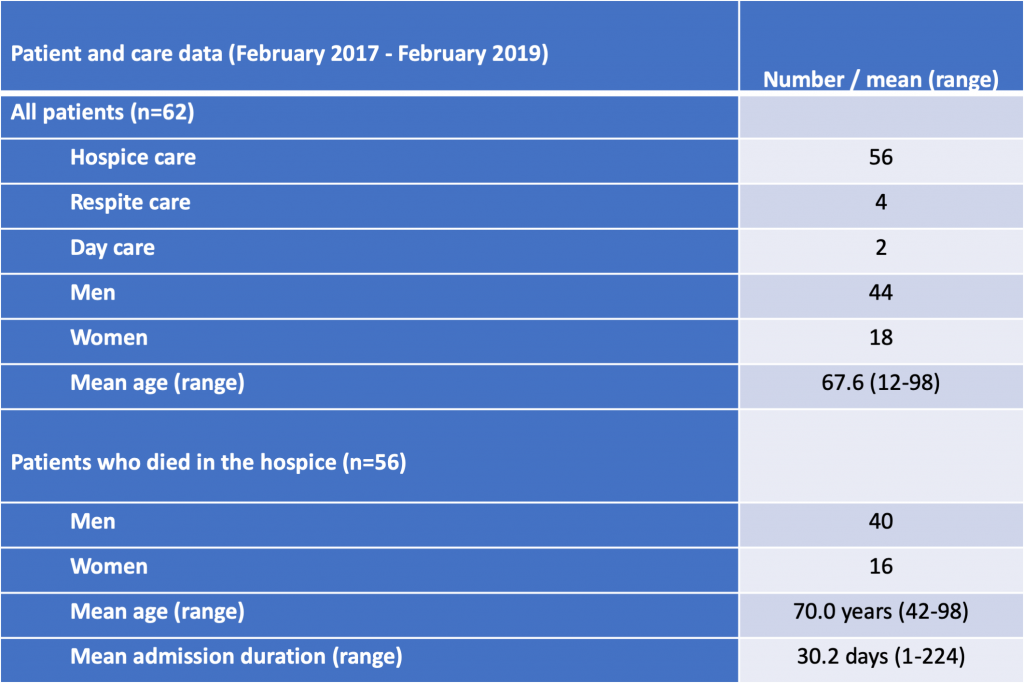
Basic patient and care data are shown in Table 1. Balade admitted a small number of patients for respite care (family relief) and day care. One patient admitted for respite care was 12; another patient admitted for day care was 25. All other patients were 42 and over. The admission duration among the patients who died in the hospice varied greatly.
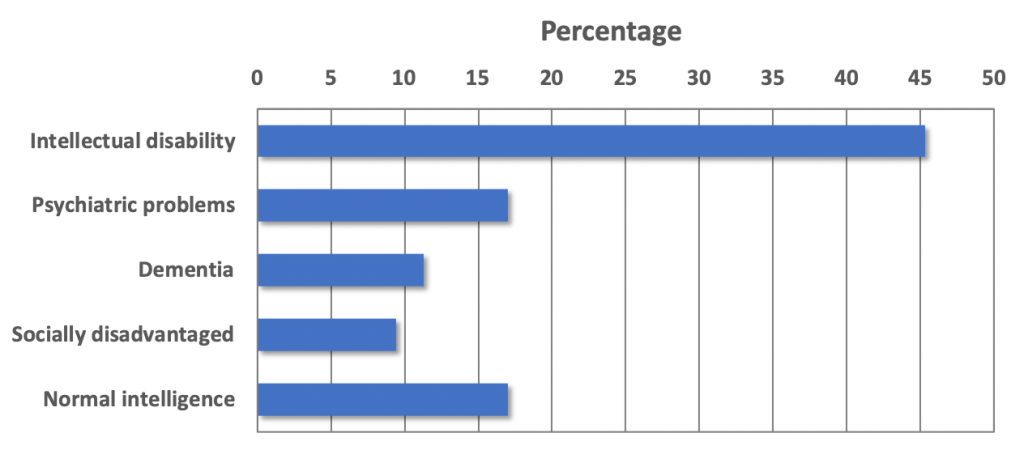
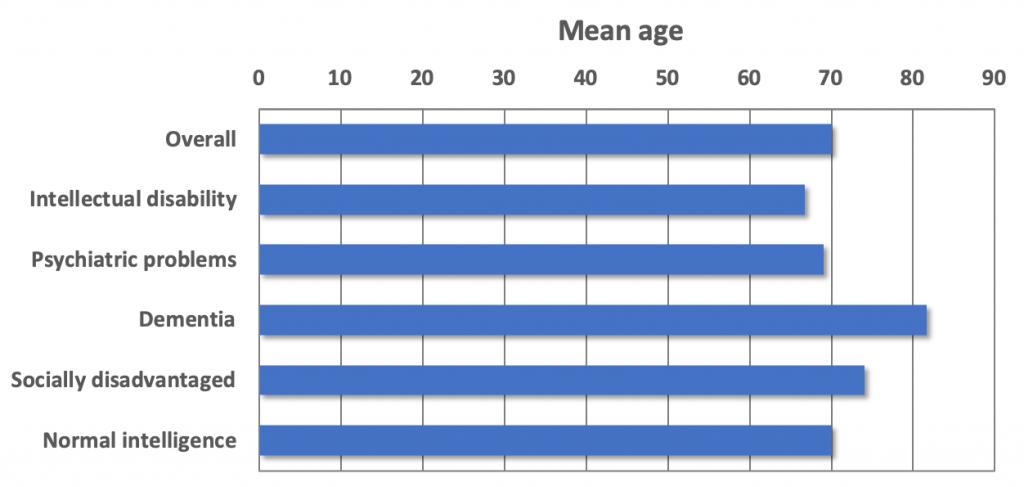
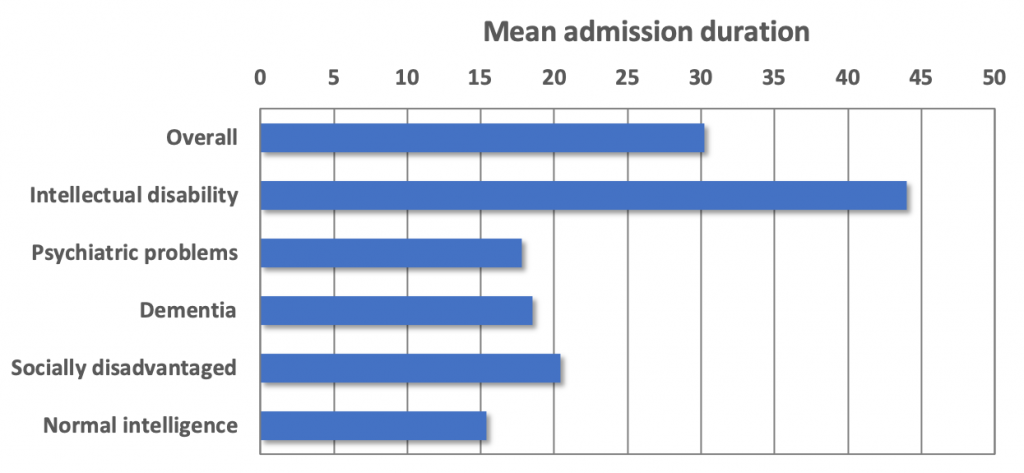
Of the 56 patients who received hospice care and who died in the hospice, most had intellectual disabilities (Chi-square=22.38, p<.01). In addition to patients with psychiatric problems, dementia and socially disadvantaged patients, patients with normal intelligence were also admitted. The distribution of patient types is shown in Figure 1. The mean age within each patient type is shown in Figure 2. Patients with dementia were oldest; patient with intellectual disabilities youngest; the differences were significant (Kruskall-Wallis H=9.89; p=.04). Figure 3 shows the mean admission duration per patient type. Patients with intellectual disabilities were admitted longer than all other patient types. The overall differences were not significant (Kruskall-Wallis H=4.62; p=.33), but the intellectual disability group against all other groups was significant (Mann-Whitney U=217.00; p=.19).
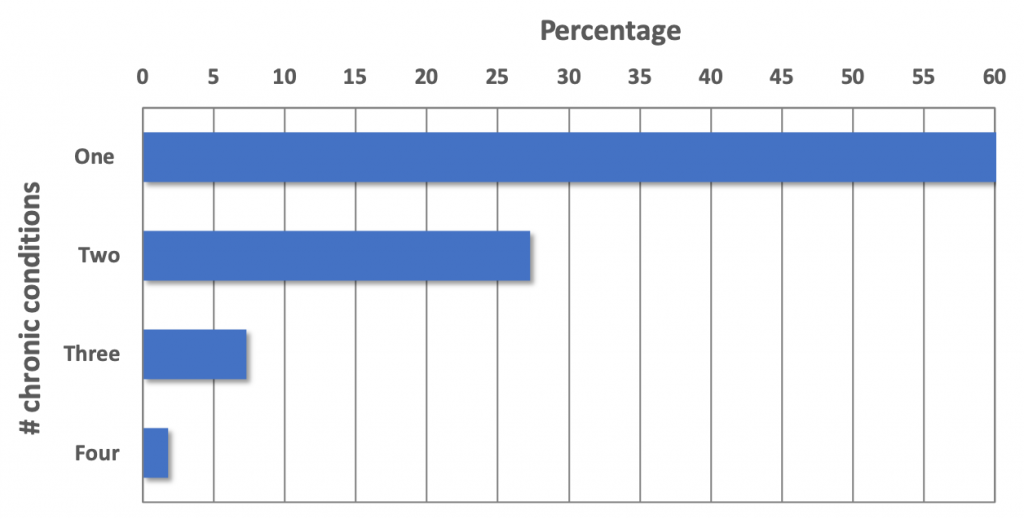
The 56 patients admitted for hospice care had various diagnoses, but most diagnoses were cancer types (Chi-square=146.27, p<.01), as shown in Figure 4. Figure 5 shows the number of concurrent diagnoses (multimorbidity). Most patients had one diagnosis (Chi-square=51.69, p<.01).

Discussion
Balade admitted patients for day care and respite care in addition to hospice care. Symptoms in all patients were controlled. Mean age was 70 years; patients with dementia were older than other patient groups. More men than women were admitted. Hospice patients were admitted for a month on average, but the rage of admission duration was large. Patients with intellectual disabilities were admitted longest. Most patients had cancer and had only one chronic diagnosis.
How do these data compare with regular hospices? The Netherlands Comprehensive Cancer Organisation (IKNL) collected data in 45 hospices in The Netherlands in 2015 (https://www.iknl.nl/over-iknl/nieuws/nieuws-detail/2016/09/12/jaarverslag-hospices-bijna-gelijk-aantal-opnameverzoeken-in-2015). There were some differences between the IKNL data and the Balade data. In the IKNL data, the mean age of the patients was 75.6 years (Balade: 70.0 years); the percentage of cancer diagnoses was 75% (Balade: 58.2%). Admission duration in the IKNL data was 28.8 days, which is in agreement with the Balade data. Lastly, IKNL did not report social work professionals being active in hospices in The Netherlands.
The Balade experiment is working. Almost all intended patient groups are being admitted to Balade. Only homeless people do not seem to be able to find their way to Balade. There are some noticeable differences with other hospices in The Netherlands, but also some similarities. In the future, cooperating with various care organisations in the area of Balade will be beneficial, especially organisations for homeless people. Balade will continue to share experiences regarding hospice care for people with intellectual disabilities, dementia, acquired brain damage, psychiatric problems, substance abuse problems and homeless people.
